Treatment
Treatment depends upon the tumour type, patient's age and general condition.
- Surgery
- Radiation Therapy
- Chemotherapy
Surgery is generally the initial and sometimes only treatment required. The aim is to remove as much of the tumour as is safely possible. Before the operation the neurosurgeon carefully studies the CT/MRI scans. The route and type of operation is then decided after discussing the risks and benefits of this operation with the patient. Hair is completely shaved before the operation. The operation is performed after giving anaesthesia to the patient. While it is desirable to remove the tumour completely, this is not always possible if the tumour is very deep-seated or is in a very critical area. Therefore a tumour may be either completely or partially removed or only a biopsy may be taken. High-powered operating microscopes make it easier to see and remove tumours while sparing the normal brain. The operation may take many hours. The patient usually wakes up as soon as the effect of the anaesthesia wears off, but is kept in the ICU for some time to allow close observation and care.
The various Neurosurgical approaches are:
Craniotomy - This is the commonest approach which allows maximum tumour removal. To reach the tumour, a window is created by cutting the skull bone and after the operation this bone is replaced.Trans Sphenoidal approach is used for removing tumours in the pituitary region by going through the nose and opening a key hole in the sphenoid sinus / base skull. Skull Base or Craniofacial approach is used for removing tumours in and around the base of the skull. Usually a team of neurosurgeons and ENT or Head & Neck surgeons perform this operation together. Stereotactic Biopsy is done for deep-seated or critically situated tumours where open biopsy is thought to be more risky. A CT or MRI scan is done with the patient wearing a stereotactic head frame. Using computers for accurate localisation, a needle is inserted through a small opening in the skull bone to take small piece of tumour tissue (biopsy) for pathological examination.
VP or VA Shunt operation is done when the tumour is blocking the flow of the cerebrospinal fluid (CSF). A long tube is inserted under the skin to divert the CSF flow from the brain ventricles to the peritoneal or atrial cavity.
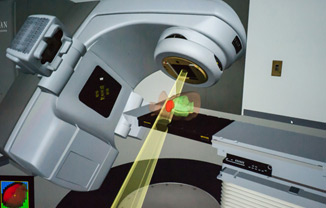 Radiation Therapy or Radiotherapy (RT) is the use of penetrating X-ray or Gamma ray beams produced by the Telecobalt or Linear Accelerator machines. Radiotherapy plays a very important role in all malignant tumours and even in some benign brain tumours. Following surgery, radiation therapy targets the remaining tumour cells to prevent or delay its recurrence. Depending upon the sensitivity of different tumour types to radiation and the biological dose of radiation used, these tumours are either completely eradicated (cured) or they shrink or stabilise thus relieving symptoms. The dose, duration and technique of radiotherapy depends upon the type, size, site of the tumour and the patient's age and general condition. For most tumours, only the affected part of the brain with some margins is irradiated. However for some tumours like medulloblastoma, lymphoma and germ cell tumours that have a higher risk of spread to the spine, the entire brain and spine is irradiated. Treatment Planning using head masks of thermoplastic material (ORFIT), simulator machines and planning computers help in more accurate positioning of the radiation beam for adequate coverage of the tumour while minimising the dose to the normal brain. After studying the CT / MRI scans, surgical and pathology reports, the area to be treated is decided. The path of the radiation beam is then carefully marked on the Thermoplastic mask using the simulator machines.
Radiation Therapy or Radiotherapy (RT) is the use of penetrating X-ray or Gamma ray beams produced by the Telecobalt or Linear Accelerator machines. Radiotherapy plays a very important role in all malignant tumours and even in some benign brain tumours. Following surgery, radiation therapy targets the remaining tumour cells to prevent or delay its recurrence. Depending upon the sensitivity of different tumour types to radiation and the biological dose of radiation used, these tumours are either completely eradicated (cured) or they shrink or stabilise thus relieving symptoms. The dose, duration and technique of radiotherapy depends upon the type, size, site of the tumour and the patient's age and general condition. For most tumours, only the affected part of the brain with some margins is irradiated. However for some tumours like medulloblastoma, lymphoma and germ cell tumours that have a higher risk of spread to the spine, the entire brain and spine is irradiated. Treatment Planning using head masks of thermoplastic material (ORFIT), simulator machines and planning computers help in more accurate positioning of the radiation beam for adequate coverage of the tumour while minimising the dose to the normal brain. After studying the CT / MRI scans, surgical and pathology reports, the area to be treated is decided. The path of the radiation beam is then carefully marked on the Thermoplastic mask using the simulator machines.
Stereotactic radiosurgery (SRS) and radiotherapy (SRT) are special techniques of radiotherapy which have the potential to reduce the dose of radiation to normal brain and critical structures as compared to conventional radiotherapy. These techniques require a lot of manpower and high technology and are indicated in special types of tumours or conditions. We are also conducting some trials in this regard (please see research in BTF).
Three dimentional conformal radiotherapy (3D-CRT) and Intensity modulated radiotherapy (IMRT) are the newer modalities of treatment delivery.These modalities are used to deliver higher dose to the target and reduce dose to adjacent critical organs. Thus they reduce normal tissue toxicity. IMRT is mainly used in tumours close to critical structures like, optic chiasm, pituitary gland, hypothalamus and in skull base tumours.
 Chemotherapy is the treatment of certain types of brain tumours with cytotoxic drugs. Chemotherapy is useful for a variety of brain tumours including lymphomas, medulloblastomas, germ cell tumours, PNET and some gliomas. Commonly used drugs used for brain tumours are CCNU, BCNU, vincristine, Cisplatin, Temozolomide etc. Generally these drugs are given in combination every 4 to 6 weeks to a maximum of 6 cycles. Sometimes, if one combination of drug regimen stops working for the tumour, another drug or a combination (2nd line) may be tried. Most of the chemotherapy treatment may be administered on an OPD basis although some may require admission. Blood tests for haemoglobin, white blood count and platelets and sometimes, liver and kidney function tests are done before each cycle of chemotherapy.
Chemotherapy is the treatment of certain types of brain tumours with cytotoxic drugs. Chemotherapy is useful for a variety of brain tumours including lymphomas, medulloblastomas, germ cell tumours, PNET and some gliomas. Commonly used drugs used for brain tumours are CCNU, BCNU, vincristine, Cisplatin, Temozolomide etc. Generally these drugs are given in combination every 4 to 6 weeks to a maximum of 6 cycles. Sometimes, if one combination of drug regimen stops working for the tumour, another drug or a combination (2nd line) may be tried. Most of the chemotherapy treatment may be administered on an OPD basis although some may require admission. Blood tests for haemoglobin, white blood count and platelets and sometimes, liver and kidney function tests are done before each cycle of chemotherapy.
Other Facilities:
Craniofacial Surgery for skull base and other tumours conducted at TMH by a team of Neurosurgeons and Head Neck surgeons. Routine neurosurgery performed at the KEM Hospital.Chemotherapy: Outapatient and Inpatient chemotherapy in a Special children's chemotherapy ward.
Rehabilitation Services: Well equipped departments with trained staff for physiotherapy, occupational therapy, speech therapy and psychological evaluation and therapy.
